Black Pigmentation on Face: Treatment Options Explained
Discover effective treatments for black pigmentation on face. Learn about laser therapy, chemical peels, and medical-grade solutions from Singapore aesthetic experts.
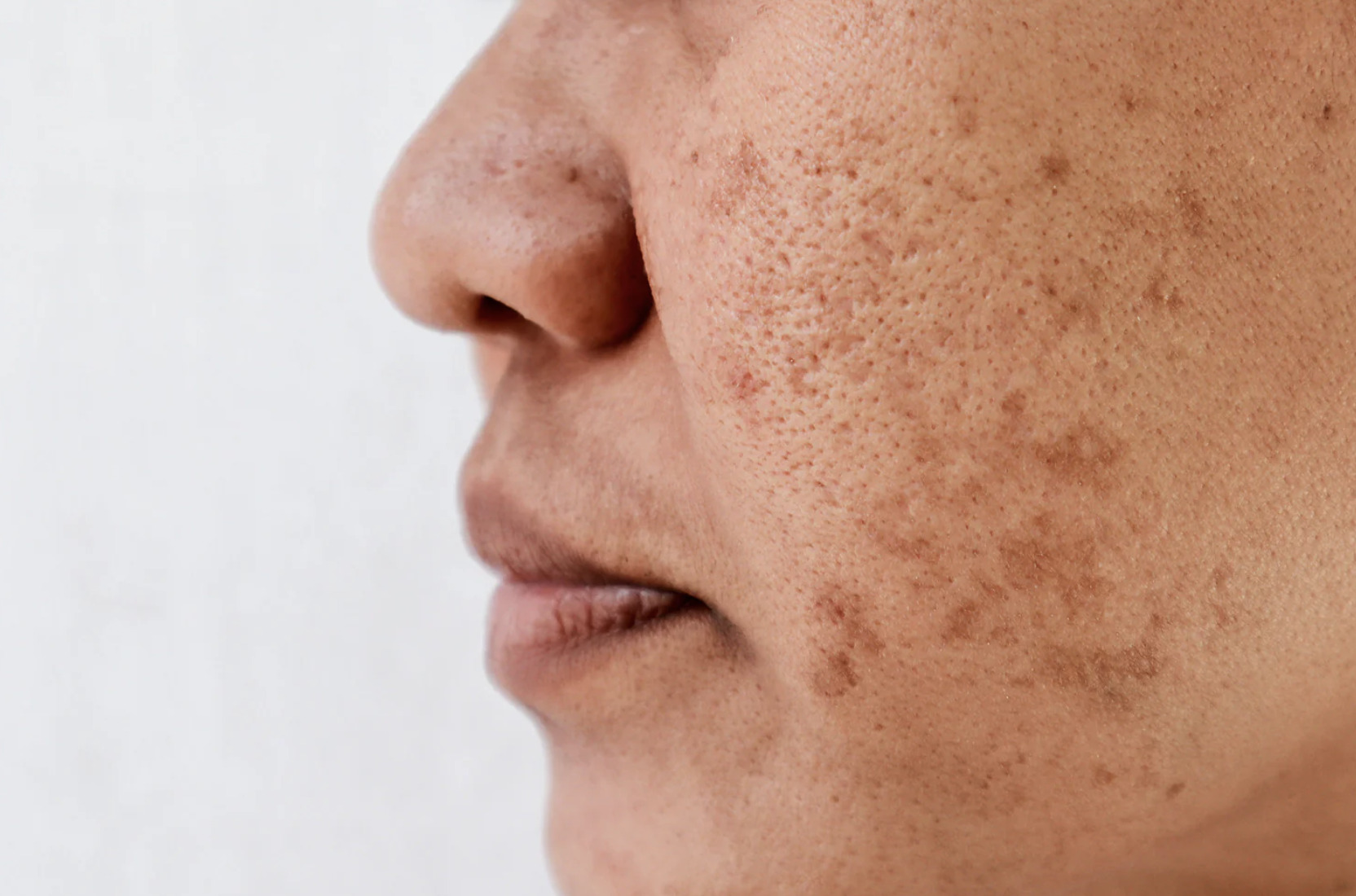
Facial pigmentation appears as darkened patches, spots, or uneven skin tone caused by excess melanin production. These changes affect the skin’s appearance in various patterns, ranging from small freckles to large patches covering significant facial areas. Treatment approaches range from topical medications to laser therapies, each targeting different pigmentation types and depths within the skin layers.
Melanin production increases due to multiple triggers, including sun exposure, hormonal changes, post-inflammatory responses, and genetic factors. The depth and distribution of excess melanin determine both the type of pigmentation and the most effective treatment approach. Surface-level pigmentation typically responds well to topical treatments, while deeper pigmentation often requires laser therapy or combination approaches.
Melasma presents as symmetrical brown or grey-brown patches, typically appearing on the cheeks, forehead, upper lip, and nose. Hormonal fluctuations during pregnancy or from oral contraceptives frequently trigger melasma development. The condition affects both the epidermis and the dermis, making treatment more complex than surface-level pigmentation.
Treatment requires a multi-pronged approach that combines sun protection, topical depigmenting agents, and, often, procedural interventions. Hydroquinone 2-4% remains the gold standard topical treatment, though tretinoin, kojic acid, and azelaic acid provide alternatives. Chemical peels using glycolic acid or trichloroacetic acid help accelerate pigment removal when combined with topical treatments.
PIH develops following skin injury or inflammation, appearing as flat spots darker than the surrounding skin. Acne, eczema, burns, and aggressive skincare treatments commonly trigger PIH. The discolouration results from melanocytes producing excess pigment during the healing process.
Darker skin types experience PIH more frequently and severely due to higher baseline melanin content. Treatment focuses on gentle exfoliation and melanin suppression using ingredients such as vitamin C, niacinamide, and alpha-hydroxy acids. Avoiding further irritation during treatment prevents worsening of existing PIH.
Solar lentigines appear as well-defined brown spots on sun-exposed areas, particularly the face, hands, and shoulders. Years of cumulative UV exposure cause melanocyte hyperactivity in localised areas. These spots typically emerge after age 40 and increase in number and size without intervention.
Q-switched lasers effectively target solar lentigines by delivering precise energy to break apart concentrated melanin. Intense Pulsed Light (IPL) treatments also reduce age spots while improving overall skin tone. Cryotherapy with liquid nitrogen is another option for isolated spots, although post-treatment hypopigmentation occasionally occurs.
Freckles manifest as small, flat brown spots that darken with sun exposure and fade during the winter months. Genetic predisposition determines freckle development, with fair-skinned individuals showing higher susceptibility. Unlike age spots, freckles appear in childhood and respond dynamically to UV exposure.
Treatment options include topical retinoids to accelerate cell turnover and broad-spectrum sunscreens to prevent darkening. Laser treatments effectively reduce the appearance of freckles, although a genetic predisposition means new freckles may develop with continued sun exposure.
Proper diagnosis begins with visual examination under natural and UV light. Wood’s lamp examination reveals pigmentation depth: epidermal pigmentation appears more pronounced under UV light, whereas dermal pigmentation shows minimal change. This distinction guides treatment selection, as superficial pigmentation responds more readily to topical agents.
Dermoscopy provides magnified visualisation of pigmentation patterns, helping to differentiate benign pigmentation from concerning lesions. Digital imaging systems document pigmentation severity and track treatment progress through standardised photography. Some clinics employ melanin-measurement devices to objectively quantify pigmentation levels.
Patient history provides important information on pigmentation triggers, duration, prior treatments, and medication use. Hormonal history, sun exposure habits, and family history of pigmentation influence both diagnosis and treatment planning.
Prescription-strength hydroquinone (4%) inhibits tyrosinase enzyme activity, reducing melanin production. Application twice daily to affected areas typically shows results within 8-12 weeks. Combination formulations containing hydroquinone, tretinoin, and corticosteroids (triple combination therapy) enhance efficacy for stubborn pigmentation.
Retinoids accelerate cellular turnover, bringing pigmented cells to the surface for faster elimination. Tretinoin 0.025-0.1% applied nightly improves pigmentation while providing anti-ageing benefits. Initial irritation is common but typically subsides as the skin adjusts to treatment.
Non-hydroquinone alternatives include kojic acid, arbutin, licorice extract, and tranexamic acid. These ingredients act through multiple mechanisms to inhibit melanin synthesis. Vitamin C serums in concentrations of 10-20% provide both pigmentation reduction and antioxidant protection.
? Did You Know?
Tranexamic acid, originally developed as an oral medication to control bleeding, shows efficacy in treating melasma when applied topically or administered through microneedling.
Superficial peels with glycolic acid (30-70%) or salicylic acid (20-30%) remove the outermost skin layers that contain excess pigment. Treatment sessions occur every 2-4 weeks, with gradual lightening observed over multiple sessions. Mandelic acid peels offer gentler exfoliation suitable for sensitive skin types.
Medium-depth peels utilising trichloroacetic acid (TCA) 15-35% penetrate deeper, addressing more stubborn pigmentation. These peels require longer downtime, with visible peeling lasting 5-7 days. Jessner’s solution combines salicylic acid, lactic acid, and resorcinol for enhanced penetration and efficacy.
Q-switched Nd: YAG lasers deliver nanosecond pulses that shatter melanin particles without damaging surrounding tissue. The 1064nm wavelength safely treats deeper pigmentation in all skin types, while the 532nm wavelength targets superficial brown spots. Treatment sessions occur monthly, with most patients requiring 3-6 sessions.
Picosecond lasers deliver ultra-short pulses measured in trillionths of a second, creating photoacoustic effects that fragment pigment more efficiently. These newer devices often achieve results with fewer treatment sessions and reduced risk of post-inflammatory hyperpigmentation.
Fractional lasers create microscopic treatment zones, leaving surrounding tissue intact for faster healing. This approach effectively treats melasma and PIH while stimulating collagen production. Non-ablative fractional lasers, such as 1927nm thulium lasers, specifically target pigmentation with minimal downtime.
IPL devices emit broad-spectrum light (500-1200nm) that targets multiple chromophores, including melanin and haemoglobin. This versatility allows simultaneous treatment of pigmentation and vascular concerns. Filter selection customises treatment for specific pigmentation types and skin tones.
Treatment protocols typically involve 3-5 sessions spaced 3-4 weeks apart. Immediate darkening of pigmented lesions occurs post-treatment, followed by gradual flaking over 7-10 days. Proper cooling and conservative energy settings minimise adverse effects.
⚠️ Important Note
IPL treatments carry higher risk of paradoxical darkening in darker skin types. Pre-treatment test spots and conservative parameters reduce this risk significantly.
Combination therapy addresses pigmentation through multiple mechanisms, enhancing overall efficacy. Topical pre-treatment with hydroquinone or tretinoin for 4-6 weeks before laser therapy improves treatment outcomes and reduces PIH risk. This approach “primes” the skin by suppressing melanocyte activity.
Sequential treatments maximise results: starting with chemical peels to address superficial pigmentation, followed by laser therapy for deeper pigmentation. Maintenance involves ongoing topical treatments and strict sun protection to prevent recurrence.
Oral tranexamic acid (250mg twice daily) combined with topical treatments shows particular efficacy for melasma. This systemic approach interrupts melanin production pathways inaccessible to topical treatments alone. Regular monitoring of liver function ensures safe long-term use.
Immediate post-treatment care varies by procedure type. Laser and IPL treatments require gentle cleansing, regular application of a moisturiser, and strict sun avoidance. Cool compresses reduce swelling and discomfort during the first 24-48 hours. Avoid picking or scrubbing treated areas as they heal.
Sun protection becomes paramount following any pigmentation treatment. Broad-spectrum SPF 50+ sunscreen applied every 2 hours during sun exposure prevents treatment reversal. Physical blockers containing zinc oxide or titanium dioxide provide protection. Wide-brimmed hats and seeking shade supplement sunscreen use.
Gentle skincare routines prevent irritation that could trigger PIH. Fragrance-free, hypoallergenic products minimise the risk of allergic reactions. Introduce active ingredients gradually, starting with alternate-day use before progressing to daily application.
Daily sunscreen application remains the cornerstone of pigmentation prevention. Apply 1/4 teaspoon to face and neck 30 minutes before sun exposure. Reapplication every 2 hours maintains protection, especially after swimming or sweating. Indoor environments with significant window exposure still require protection.
Antioxidant serums containing vitamin C, vitamin E, and ferulic acid neutralise free radicals that trigger melanin production. Applying sunscreen in the morning provides dual protection against UV damage and oxidative stress.
Hormonal management helps prevent melasma recurrence. Discussing alternative contraceptive methods with healthcare providers may benefit those with hormone-triggered pigmentation. Pregnancy-related melasma often requires modified treatment approaches using pregnancy-safe ingredients.
“Facial pigmentation treatment success depends on accurate diagnosis and customised treatment protocols. At a medical aesthetic clinic in Singapore, many patients benefit from combination approaches rather than relying on single treatments. I emphasise the importance of realistic expectations, while significant improvement is achievable, complete elimination isn’t always possible, especially with melasma.
The success lies in identifying triggering factors and addressing them alongside active treatment. Patients who commit to daily sun protection and maintenance treatments achieve sustainable results. Modern laser technology allows us to treat various skin types safely, though careful parameter selection remains important.”
How long before I see results from facial pigmentation treatment?
Topical treatments typically show initial improvement within 4-6 weeks, with results at 12-16 weeks. Laser treatments often produce visible lightening after 2-3 sessions, though some experience temporary darkening immediately post-treatment. Chemical peels show gradual improvement over multiple sessions spaced 2-4 weeks apart.
Can facial pigmentation return after successful treatment?
Recurrence of pigmentation depends on the underlying cause and maintenance efforts. Melasma frequently recurs without ongoing treatment and sun protection. Solar lentigines may develop new spots with continued sun exposure. Consistent sunscreen use and maintenance treatments significantly reduce recurrence rates.
Which treatment works fastest for facial pigmentation?
Laser treatments typically produce the fastest visible results, particularly for discrete lesions such as solar lentigines. However, aggressive treatments risk causing PIH. Treatment selection should prioritise safety and sustainability over speed.
Is facial pigmentation treatment safe for all skin types?
Modern treatments can safely address pigmentation in all skin types when properly selected and performed. Darker skin requires modified protocols with conservative energy settings and longer treatment intervals. Pre-treatment with topical agents and test spots minimises adverse effects.
What’s the difference between IPL and laser for pigmentation?
Lasers emit single-wavelength light, providing precise targeting of specific pigment depths. IPL uses broad-spectrum light affecting multiple targets simultaneously. Lasers generally yield more consistent results for specific lesions, whereas IPL addresses diffuse pigmentation and overall skin tone.
Effective skin pigmentation treatment in Singapore starts with a detailed professional assessment to determine the cause, type, and depth of pigmentation. Combining medical-grade treatments with consistent skincare and sun protection often achieves the best results and long-term improvement.
If you’re experiencing persistent facial pigmentation that affects your confidence, our aesthetic doctors can provide a comprehensive evaluation and customised treatment plan tailored to your skin’s needs.

Every patient is important to me! The most delightful aspect of my profession is to see the satisfaction of my patients and the biggest earning in my career is the patients trust on me.
Dr. Sam has many years of experience in the aesthetic medicine and has worked with industry professionals for more than a decade.
After obtaining his Bachelor of Medicine and Bachelor of Surgery (MBBS), his experience in Anaesthesia, ICU management, Chronic pain management have laid a solid foundation in understanding & managing the pain during aesthetic procedures in a safe and effective manner.
Dr. Sam’s Passion and desire in aesthetic medicine made him to work hard in mastering skills & obtaining required certifications to become an aesthetic physician.

Fill up the form and we will get back to you as soon as possible.