HIFU Forehead Tightening in Singapore: What You Should Expect
HIFU forehead tightening treatment process, recovery in Singapore.
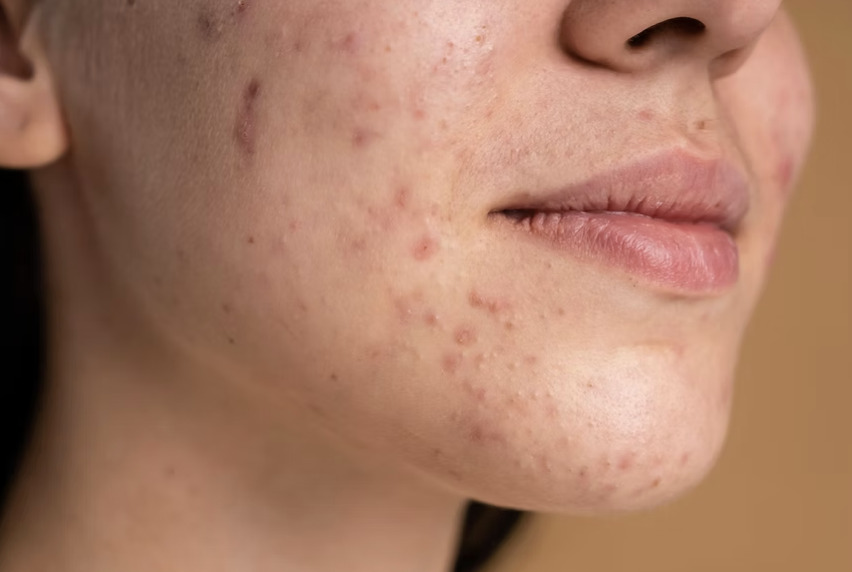
Chin acne differs from facial acne elsewhere due to its hormonal connections and tendency toward deep, painful cysts. The chin and jawline contain dense sebaceous glands that respond strongly to hormonal fluctuations, making this area particularly prone to persistent breakouts. Treatment requires addressing both the visible acne and its underlying hormonal triggers.
The location of chin acne presents unique challenges. Unlike forehead or cheek acne, chin breakouts often resist standard topical treatments due to thicker skin in this area and constant irritation from touching, phone contact, and mask-wearing.
Hormonal fluctuations drive most cases of chin acne. At a medical aesthetic clinic in Singapore, androgens are commonly identified as a key trigger, as they stimulate sebaceous glands along the jawline, increasing oil production and creating ideal conditions for acne-causing bacteria. Many women notice chin breakouts that align with menstrual cycles, often worsening during the luteal phase when progesterone levels rise.
The chin area also harbors specific bacteria strains that thrive in oxygen-poor environments. Within hair follicles, Cutibacterium acnes proliferates rapidly when excess sebum blocks pores. This bacterial overgrowth triggers inflammatory responses, leading to the painful, deep cysts typically associated with hormonal chin acne.
Physical factors further compound the issue. Frequent hand-to-face contact transfers bacteria from hands to the face, while phone screens can harbor large numbers of microorganisms. Mask-wearing creates a humid environment that traps oil and bacteria against the skin. Musical instruments, chin straps, and scarves add friction and increase bacterial transfer.
Hair products also contribute significantly to acne on the chin. Oils, waxes, and silicones in styling products can migrate down the face during the day, clogging pores along the jawline. Toothpaste containing sodium lauryl sulfate may irritate the skin around the mouth, triggering breakouts along the chin and perioral area.
Retinoids remain the standard for the treatment of chin acne. Tretinoin accelerates cell turnover, preventing dead skin cells from clogging pores while simultaneously reducing inflammation. Starting with 0.025% concentration and gradually increasing helps minimize irritation. Apply pea-sized amounts to clean, dry skin, avoiding the immediate eye area.
Benzoyl peroxide kills acne bacteria through oxidation, making it particularly effective for inflammatory chin acne. The 2.5% concentration provides antibacterial benefits with less irritation than higher strengths. Layer benzoyl peroxide over moisturizer to reduce dryness, especially during the initial weeks of treatment.
Azelaic acid offers dual benefits: antimicrobial action and anti-inflammatory properties. The 15-20% prescription formulations work well for chin acne, particularly in patients with darker skin tones who risk post-inflammatory hyperpigmentation. Apply twice daily after cleansing for results.
Topical antibiotics, such as clindamycin, directly target bacterial overgrowth. However, using antibiotics alone increases the risk of resistance. Combining clindamycin with benzoyl peroxide in formulations such as Duac or BenzaClin prevents resistance while maximizing antibacterial efficacy.
Oral antibiotics are indicated for moderate to severe chin acne when topical agents are insufficient. Doxycycline and minocycline reduce both bacteria and inflammation. Sub-antimicrobial doses (40mg doxycycline daily) provide anti-inflammatory benefits without promoting resistance. Treatment typically continues for 3-4 months before reassessment.
Hormonal treatments effectively target the root cause of chin acne in women. Combined oral contraceptives containing ethinyl estradiol with anti-androgenic progestins (like drospirenone or norgestimate) reduce sebum production. Results typically appear after 3-6 months of consistent use.
Spironolactone blocks androgen receptors, decreasing hormonal stimulation of sebaceous glands. Starting doses of 25-50mg daily minimize side effects while providing anti-acne benefits. Most patients require 100-150mg daily for chin acne control. Regular potassium monitoring ensures safety during treatment.
Isotretinoin is used to treat severe, treatment-resistant chin acne. This vitamin A derivative reduces sebaceous gland size and normalizes skin cell turnover. Treatment courses typically last 5-6 months, with dosing based on body weight. Monthly monitoring of liver function and lipid levels is performed throughout treatment.
Salicylic acid peels penetrate oil-filled pores effectively, making them ideal for chin acne. The 20-30% concentrations used in clinical settings dissolve dead skin cells and reduce inflammation. Treatments occur every 2-4 weeks until desired improvement, with minimal downtime between sessions.
Glycolic acid peels address both active acne and post-inflammatory marks. Starting with 30% concentration and progressing to 70% based on tolerance helps resurface skin while stimulating collagen production. The chin’s thicker skin tolerates higher concentrations than other facial areas.
Blue light therapy targets acne bacteria using specific wavelengths (415nm) that trigger bacterial self-destruction. Sessions last 15-20 minutes and are performed twice weekly for 4-6 weeks. LED devices provide gentler treatment than traditional photodynamic therapy, with no downtime required.
Pulsed-dye lasers reduce inflammation and redness associated with acne on the chin. The 595nm wavelength targets blood vessels feeding inflamed lesions, accelerating healing. Single treatments address individual cysts, while a series of 3-4 sessions improves overall skin texture.
Professional extractions remove stubborn comedones safely. Dermatologists use specialized tools and techniques to minimize trauma and scarring risk. Pre-treatment with retinoids softens comedones, facilitating easier extraction.
Intralesional corticosteroid injections rapidly reduce the size of painful chin cysts. Triamcinolone acetonide (2.5-5mg/ml concentration) injected directly into cysts reduces inflammation within 24-48 hours. Multiple injections spaced 4-6 weeks apart may be needed for recurring cysts.
Double cleansing removes makeup, sunscreen, and accumulated oils without stripping skin. Start with micellar water or cleansing oil to dissolve oil-based impurities. Follow with a gentle, pH-balanced gel cleanser to remove remaining residue. Avoid harsh surfactants that compromise skin barrier function.
Cleansing tools require careful selection and maintenance. Soft silicone cleansing pads provide gentle exfoliation without harboring bacteria. Replace traditional washcloths daily or use disposable options to prevent bacterial recontamination. Sonic cleansing devices help dislodge debris from pores when used with appropriate pressure.
Spot treatments containing sulfur dry individual blemishes overnight. The 10% sulfur concentration draws out excess oil while reducing bacterial growth. Apply directly to clean skin before applying a moisturizer, avoiding the surrounding areas to prevent excessive dryness.
Clay masks formulated with kaolin or bentonite absorb excess sebum from the chin area. Weekly applications help prevent pore congestion without over-drying. Focus application on oily zones; leave masks on for a maximum of 10-15 minutes.
? Did You Know?
The chin contains fewer oil glands than the forehead but produces thicker sebum, making blockages more likely to form deep, painful cysts rather than surface whiteheads.
Diet modifications may improve chin acne in some individuals. Reducing high-glycemic foods and dairy products helps stabilize insulin levels that influence sebum production. Increasing omega-3 fatty acid intake through fish consumption or supplements confers anti-inflammatory benefits.
Stress management directly impacts hormonal balance. Cortisol elevation triggers increased androgen production, exacerbating acne. Regular exercise, adequate sleep (7-9 hours nightly), and stress-reduction techniques help regulate hormone levels naturally.
Phone hygiene prevents bacterial transfer to the chin area. Daily cleaning with alcohol wipes removes accumulated bacteria and oils. Using speakerphone or headphones minimizes direct skin contact during calls.
Non-comedogenic products prevent pore blockage without sacrificing efficacy. Look for lightweight, gel-based moisturizers containing hyaluronic acid or glycerin. Avoid heavy creams containing occlusive agents such as petrolatum or mineral oil on the chin.
Exfoliation helps maintain clear pores when performed correctly. Chemical exfoliants (BHAs) are more effective than physical scrubs for acne on the chin. Use 2% salicylic acid treatments 2-3 times weekly, adjusting frequency based on skin tolerance.
Sun protection requires careful product selection. Mineral sunscreens with zinc oxide or titanium dioxide provide broad-spectrum protection without clogging pores. Apply generously to the chin area, reapplying every 2 hours during sun exposure.
Hormonal awareness helps anticipate and prevent cyclic breakouts. Track menstrual cycles alongside acne flares to identify patterns. Increase preventive treatments during high-risk weeks, such as adding benzoyl peroxide or increasing retinoid frequency.
Chin acne often requires combination therapy for results. I typically start patients on topical retinoids with antimicrobial agents, adding oral medications if improvement plateaus after 8-12 weeks. The approach is to address both acne and its hormonal triggers simultaneously.
Many patients underestimate the importance of consistent treatment. Chin acne responds slowly due to deep-rooted cysts and hormonal influences. I counsel patients to expect 3-4 months before seeing significant improvement, with maintenance therapy continuing indefinitely to prevent recurrence.
Professional treatments complement home care rather than replacing it. Chemical peels and extractions provide immediate improvement, but daily skincare maintains these results. I recommend professional treatments every 4-6 weeks during active breakout phases, spacing them further as skin improves.
How long does chin acne treatment take to work?
Most topical treatments require 6-12 weeks of consistent use before showing significant improvement. Oral medications, such as antibiotics, may show results within 4-6 weeks, whereas hormonal treatments require 3-6 months. Professional treatments provide immediate improvement for individual lesions but require multiple sessions for lasting results.
Can I treat hormonal chin acne without medication?
Mild hormonal chin acne may respond to consistent topical care, dietary modifications, and stress management. However, moderate to severe cases typically require prescription medications to address underlying hormonal imbalances effectively. Professional guidance helps determine whether lifestyle changes alone suffice for your specific situation.
Why does chin acne leave scars more often?
Chin acne tends to form deep, inflammatory cysts that damage the surrounding tissue. The chin’s thicker skin and tendency to pick at painful lesions increase the risk of scarring. Early treatment of inflamed cysts and avoidance of manipulation reduce permanent marking.
Can men develop hormonal chin acne?
Yes, men experience hormonal chin acne, particularly during adolescence or when using testosterone supplements. Male hormonal acne typically presents as deep, painful nodules along the jawline. Treatment approaches remain similar, though hormonal medications like spironolactone aren’t appropriate for men.
Will chin acne return after isotretinoin treatment?
While isotretinoin provides long-term remission for many patients, hormonal chin acne may recur due to ongoing hormonal fluctuations. Maintenance therapy with topical retinoids or hormonal agents helps prevent recurrence after completion of isotretinoin courses.
Effective care for chin acne combines appropriate medical interventions with consistent daily routines. Whether using topical medications, oral therapies, or in-clinic procedures such as lasers, addressing both active breakouts and root causes supports lasting improvement. Starting early helps prevent scarring and shortens overall treatment time.
If you’re experiencing persistent chin acne despite home care, our aesthetic doctors can provide a comprehensive evaluation and a customised plan that may include acne laser treatment in Singapore alongside evidence-based therapies.

Every patient is important to me! The most delightful aspect of my profession is to see the satisfaction of my patients and the biggest earning in my career is the patients trust on me.
Dr. Sam has many years of experience in the aesthetic medicine and has worked with industry professionals for more than a decade.
After obtaining his Bachelor of Medicine and Bachelor of Surgery (MBBS), his experience in Anaesthesia, ICU management, Chronic pain management have laid a solid foundation in understanding & managing the pain during aesthetic procedures in a safe and effective manner.
Dr. Sam’s Passion and desire in aesthetic medicine made him to work hard in mastering skills & obtaining required certifications to become an aesthetic physician.

Fill up the form and we will get back to you as soon as possible.